 Aimee Moore
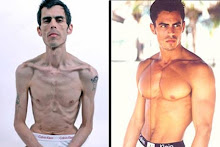
Aimee Moore Aimee Moore's mother has watched her child battle eating disorders for 15 years, a pattern of behaviour that had her daughter purge as often as 150 times a day and become a skeleton with skin
Aimee Moore's mother has watched her child battle eating disorders for 15 years, a pattern of behaviour that had her daughter purge as often as 150 times a day and become a skeleton with skin
Aimee Moore
"Aimee Moore, the Stratford woman with an extreme eating disorder, is now seeking intravenous feeding to nourish her starving body.
Moore, who spent seven weeks in an Alabama treatment facility after being featured on the Dr. Phil show, has continued to battle anorexia and bulimia since her early departure from the facility April 10.
She recently began investigating options for intravenous feeding after learning from doctors that little else can be done to treat gastroparesis, a digestive disorder which causes her extreme pain when she eats normally.
Medication hasn't been effective.
"It took me a while to process everything they were trying to tell me, but they convinced me I need this," the 68-pound Moore said last week.
With gastroparesis, the stomach takes too long to empty its contents, because of damage to a nerve which controls the movement of food from the stomach through the digestive tract."
~~~~~~~~~~
"Anonymous said...
I am the Anonymous with the anorexic granddaughter. She, too, suffers from gastroparesis and is in constant pain from the tiniest spoonfuls of food. She spent 6 months or more on intravenous, then had a feeding tube installed. Now she's staying alive on a babyfood jar of pears in a week, a supernutrient solution ($1000 per week) introduced 3-4 times daily, and an unlimited supply of CANDY to keep her blood sugar from crashing and her going into a coma. But the N.D. seems to be helping, and she does want to live. Hopefully it isn't already too late.
May 26, 2008 5:52 PM"
The following is a description of gastroparesis from the Mayo Clinic:
Gastroparesis
 Stomach
Stomach
Your stomach is a muscular sac located in the upper middle of your abdomen, just below your ribs. If you're an average adult, it's about the size of a small melon, but can stretch to hold nearly 1 gallon of food and liquid. Your stomach folds in on itself when it's empty and expands when you eat or drink.
The walls of your stomach are lined with three layers of powerful muscles that mix food with enzymes and acids produced by glands in your stomach's inner lining. Once the food is thoroughly pulverized — reduced to the consistency of porridge — strong muscular contractions (peristaltic waves) push it toward the pyloric valve, which leads to the upper portion of your small intestine (duodenum), where the real work of digestion takes place. The valve opens just enough to release a scant eighth of an ounce of food at a time.
It may take three to four hours for your stomach to empty after you eat, depending on your diet — foods high in fat can prolong the emptying time considerably. The slowness of the process ensures that food is thoroughly mixed with digestive juices for the best possible absorption.
Why the stomach stops working
Arguably the most important nerve in your body, the vagus nerve stretches from your brainstem to your colon. It helps orchestrate the complex microcircuits in your digestive tract, including signaling the smooth muscles in your stomach to contract in peristaltic waves — usually at the rate of about three contractions a minute. When these contractions slow or stop completely, food doesn't move out of your stomach into the duodenum as it should.
Damage to the vagus nerve is the leading cause of gastroparesis, although the disorder can also result from damage to the stomach muscles themselves. Factors that can damage nerves or muscles in your stomach include:
Diabetes
Affecting people with either type 1 diabetes or type 2 diabetes, this is one of the most common causes of gastroparesis. Over time, high blood glucose levels and their metabolic effects can damage the vagus nerve and disrupt its normal functioning. Once gastroparesis develops, diabetes often becomes worse because erratic stomach emptying and poor absorption make blood sugar levels harder to control.
Surgery
Operations involving your esophagus, stomach or upper part of your small intestine can injure the vagus nerve and lead to gastroparesis. Symptoms may develop immediately after the surgery or appear years later.
Medications
Many commonly prescribed drugs slow stomach emptying. Chief among these are narcotic pain medications, tricyclic antidepressants and calcium channel blockers. Antacids that contain aluminum hydroxide, some high blood pressure medications and the psychiatric drug lithium also can disrupt the normal functioning of the stomach. Symptoms usually improve once you stop taking the medication.
Cancer treatments
Nausea and vomiting are common side effects of chemotherapy because most anti-cancer drugs target fast-growing cells throughout your body, including healthy cells in your intestinal tract. The nausea and vomiting are usually temporary and improve when treatment ends.
But some people receiving high doses of chemotherapy drugs may develop intractable nausea and vomiting as a result of chemotherapy-induced gastroparesis. In that case, problems with the stomach being able to move food (motility problems) originate in the nausea center of the brainstem, just above the spinal cord. Radiation therapy to the chest and abdomen also can cause gastroparesis.
Other disorders
A number of other medical conditions can cause gastroparesis, including anorexia and bulimia, the connective tissue disease scleroderma, Parkinson's disease and other nervous system illnesses, and metabolic disorders such as hypothyroidism. For reasons that aren't clear, some otherwise healthy people develop gastroparesis after a bout of the flu or other viral illness.
By Mayo Clinic Staff
~~~~~~~~~~
My heart goes out to both Anonymous's granddaughter and Aimee Moore, and to all those suffering from gastroparesis. It is a horrific disorder.
LINKS:
http://news.therecord.com/article/329264
http://news.therecord.com/printArticle/336239
http://news.therecord.com/article/338098
http://news.therecord.com/News/Local/article/356100
http://www.mayoclinic.com/health/gastroparesis/DS00612/DSECTION=3
Follow on Buzz




























5 comments:
The following comment was posted on my mirror blog on Healthcare.com
(http://blogs.healthcare.com/medusa)on a copy of this post. Because it is so important, I am posting it here:
"Comment by LifE AbUnDaNtlY!!! on August 13, 2008 @ 9:32 am | Edit This
My sympathy & heart fully goes out to anybody who has someone close to them go through an eating disorder. Even more so, my heart extends to the individual who is dealing with it herself.
I myself know from experience….being anorexic and bulemic for years, developed gastroparisis, then I became a compulsive overeater b/c I knew I could eat anything I wanted & throw it up. With endless cycles of bad eating habits and a wacked out & obsessive mind I finally realized I hated the life I was living, in need of help, and admitted myself to Remuda Ranch, AZ. (highly recommended!!!)
Today…after years of battling with recovery I can finally say that I am FREE from the battle & addiction to eating disorders that nearly took my life! My mind is practically new—-not having to deal with the overpowering thoughts of weight, food, and depression. I have permanently damaged my stomach b/c of the disorder and to this day still deal with gastroparisis. But I will tell you, if you can get past the eating disorder & “mind” issues….gastroparisis is nothing compared…it’s only a SMALL part of it.
There is one thing I can tell you! (ok…maybe more than one thing) :)….& it is this….keeping praying, being there, and loving the one that is dealing with the disorder. I honestly believe it is by the prayers & support of those around me, I am alive to day. There is hope! Don’t lose sight of it…along as they are alive, there is hope! In terms of gastroparisis….non creamy, non fiberous, not raw foods are the best.
KEEP HOPING PRAYING> SUPPORTING> LIVING> there is hope & there is a God who can work in the midst of the craziest storms."
I am a mom of my 25 year old daughter who has gasteoparisis and stomach migranes.
My daughter cannot work and none of the current medications are helping her.
I have lost sight as to how many medications she is on. She has had so many. She struggles to try to do yoga which she can on do occassion,and because she is in so much pain we do no know what to do. Her boyfriend does not work and both are hard to help as neither of them work as he looks after her. Should we convince her to hospitalize herself into the phsycriatric ward for monitoring?
Urine therapy is beneficial for that.
Hi, I sympathize with you on this issue. Gastroparesis is a terrible disorder and is hard to manage. I was diagnosed 8 years ago after 2 years of pain sickness and numerous tests. I stopped work my life went down hill, I was depressed and suffering from anxiety. I have my symptoms under control by completely modifying my diet, I eventually cut out everything. Medications did not helo, I was trialled on many. I now eat an extremely small amount of food and have compact protein supplements by nutria. I have flare uos and then stop eating for a few days only taking juice + protein sups. I have found the most effective way to deal with this disease is by diet,taking care to not become constipated as this is a killer with gastroparesis. I use the laxative that is used by nursing homes as this causes the least amount of pain and complications. No fat in my diet, pureed babyfood in the way of apple pear banana. Hardly any fibre which complicates things as I also have diverticular disease and normally need high fibre diet to aid with this. I also have achalasia. All in all seek help from councelling if you can to aid the psychological side and be extremely strict with diet. Keep a food diary, exercise is very important too as it aids digestion.
I almost list the plot long ago because of this disease however I am still here, have a great part time job, manage my family ok and am doing much better. You will get through this as I did, it won't go away but you will be able to manage after careful modification of diet exercise and also try meditation, it's good for all aspects and you can do this free by downloading an app.
I do hope this helps :)
Don't let this disease beat you !
Gastroparesis can be caused by bulimia or AN bp subtype, longterm, in a lot of different ways...
You can damage vagus nerve through herniation in purging. You can damage nerves (generally) through longterm blood sugar dysregulation (like in diabetes, but without diabetes) if youre bping and restricting. You can cause nerve damage through electrolyte-imbalance induced strokes.
You can causes nerve damage in stomach walls through severe, repeating distention if it's done beyond a certain point-- this happens to competitive eaters, which was how i learned about it. There's not much study done on competitive eaters, but nerve damage leading to gastroparesis is the endpoint. In "normal" overeating, the person stops at the point of nausea reflexes / senses from eating too much, but in those who are longterm bulimics/AN bp/competitive eaters, many of us have blown past that point and destroyed the feedback loop.... When you repeatedly eat past that point, the vomit reflex from overeating goes away entirely (along w/ other nerve functions- satiety cues, peristalsis...) source:
http://www.ajronline.org/doi/abs/10.2214/AJR.07.2342#/doi/full/10.2214/AJR.07.2342 ... Unfortunately, unlike some body things, nerves are NOT quick to repair themselves.
While this article talks about "the hell of gastroparesis" it doesnt talk much about what that means in daily life besides pain after eating anything (except maybe semifluids). It isnt only a problem when youre awake- from gastroparesis, ive had years of sleep-maintenance insomnia, because i wake up uncomfortable from undigested food that cant exit. The only relief is in purgeing, once gastroparesis is flaring. I cannot explain how much it reinforces the binge-purge cycle.
Gastroparesis makes eating so, so much worse if you have an ED history, because all your most trusted foods are the ones who cant exit your stomach with any reliable timeframe... I always was ok w/ bigger portion of nonterrifying foods than eating things im scared of-- gastroparesis takes away that choice from you. Even a small portion of cooked vegetable/fruit might not exit your stomach for a long, long time. No more salads- the only vegetables i can do raw are like tomatoes or peeled cucumber. For a few years, a diet based heavily on smoothies and coffee and protein powders and purees is fine, but it gets old, and if you stop, the pain is severe and youre set up to get other digestive complications.
Gastroparesis in ED patients can be correlated w/ general peristalsis issues. Meaning that stomach emptying may not be the only issue- there may be intestinal peristalsis insufficiency as well. For that, if you have it, you'll need constant osmotic laxatives- forever.
Post a Comment